Before diving into the concept of computer-assisted surgery, we need to make a philosophical distinction that will guide our understanding throughout this course: the difference between Surgery and Intervention.
But What Is Surgery?¶
According to the Oxford English Dictionary, the definition of the word Surgery includes, among others:
The art or practice of treating wounds, fractured bones, and other conditions by manual operation or instrumental appliances; surgical treatment
Surgery of Access
These definitions reveal something important: surgery is fundamentally about access -- creating pathways to reach surgical targets that would otherwise be inaccessible. Consider a hepatectomy procedure as an example. Possible surgical approaches include:
If you’re having open surgery, your surgeon will make one long incision across your abdomen to open your abdominal cavity. If you’re having laparoscopic surgery, your surgeon will make 4 to 6 “keyhole” incisions, which they’ll use to place the camera (laparoscope) and surgical instruments to do the operation.
Both approaches are focused entirely on access, providing two essential elements: visualization (so surgeons can see the target, via direct human vision or indirect medical imaging) and manipulation (so surgeons can reach the surgical target with instruments).
The Evolution of Surgical Access¶
Traditional open surgery requires large incisions to establish direct line-of-sight visualization (i.e., direct human vision) and unrestricted surgical instrument access.
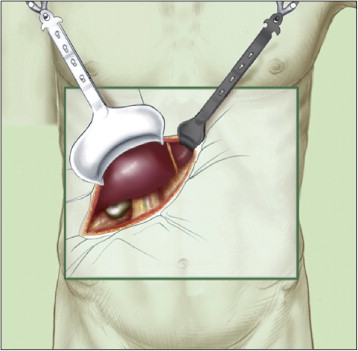
Figure 1:A depiction of open liver surgery with large incision, image courtesy of Gaujoux & Goéré (2011).
However, advances in medical imaging and mechatronics have revolutionized this approach. Technologies such as laparoscopic cameras, fibre-optic illumination, miniaturized instruments, and medical robotics now enable surgeons to achieve nearly equivalent visualization and manipulation through small keyhole incisions, forming the foundation of Minimally Invasive Surgery (MIS).
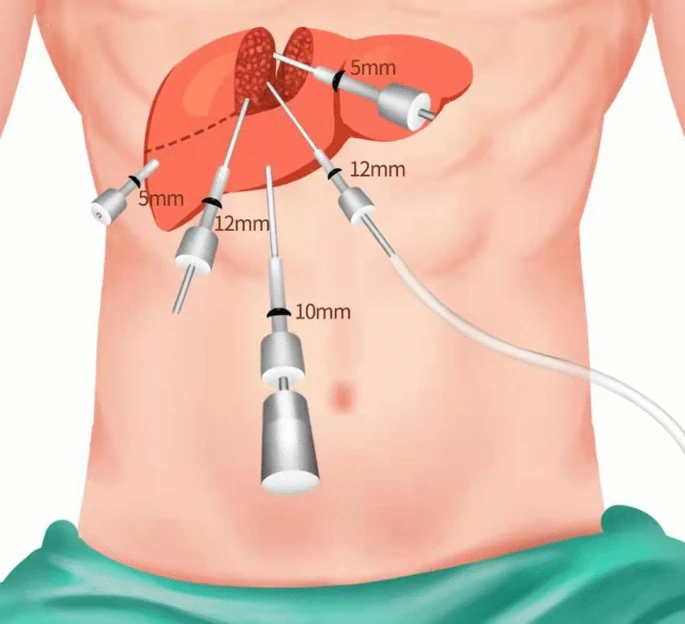
Figure 2:A depiction of MIS where surgical access is provided through trocar, image courtesy of citation Hou et al. (2022).
From an engineering perspective, this evolution represents an optimization problem: how do we maintain surgical capability while minimizing tissue trauma? The answer lies in advancing medical imaging systems, precision mechanics and mechatronics, and human-computer interfaces (HCI) that extend the surgeon’s sensory and motor capabilities.
Surgery vs. Intervention: The Critical Distinction¶
In this course, we therefore make the critical distinction between surgery and intervention:
Surgery = The means of providing surgical access to anatomical targets (e.g. exposing a tumour hidden beneath organ surfaces), and
Intervention = The therapeutic act that directly improves the patient’s condition (e.g. removing the tumour via resection or destroying it via thermal ablation).
This distinction appears across all surgical specialties:
Cardiac surgery: sternotomy (surgery) enables heart valve replacement (intervention)
Neurosurgery: craniotomy (surgery) enables brain tumour resection (intervention)
Orthopaedics: arthroscopy (surgery) enables meniscus repairs (intervention)
Implications for Computer-Assisted Surgery¶
This framework has profound implications for how we approach computer-assisted surgery technologies:
Navigation and Guidance Systems primarily assist with the surgical component - helping surgeons plan optimal access routes, tracking instrument positions, and navigate safely to targets while avoiding critical structures.
Robotic Systems can enhance both components - providing tremor-free access through constrained space (surgery) while enabling precise manipulation during the actual therapeutic interventions.
Imaging Technologies serve both functions - preoperative imaging modalities guide surgical planning and access, while intraoperative imaging modalities monitor the intervention itself.
The Philosophical Insight¶
Understanding this distinction between surgery and intervention leads to the following realization: surgery is, in fact, a side-effect of therapy!
The research problem we wish to address, in this regard, is how to deliver therapeutic interventions without any, or minimal, surgical trauma to the patient. Every incision or every tissue manipulation represents a necessary compromise - a side-effect we accept to enable outcome-improving interventions.
This perspective explains why CAS technologies are so compelling: they promise to minimize the surgical side-effects while maximizing therapeutic precision. As biomedical engineers, our goal is not just to make surgery more precise, but to make it less necessary — to find ways to deliver therapeutic interventions with minimal surgical trauma.
This conceptual framework will guide our exploration of image-guided interventions (IGI), robotic systems, and emerging technologies (such as 3D visualization) that continue to push the boundaries of what’s possible in minimally invasive intervention.
- Gaujoux, S., & Goéré, D. (2011). Surgical approach for hepatectomy. Journal of Visceral Surgery, 148(6), e422–e426. 10.1016/j.jviscsurg.2011.09.015
- Hou, Z., Xie, Q., Qiu, G., Jin, Z., Mi, S., & Huang, J. (2022). Trocar layouts in laparoscopic liver surgery. Surgical Endoscopy, 36(11), 7949–7960. 10.1007/s00464-022-09312-9